Hypertensive Crisis: What It Is and Why It’s Serious
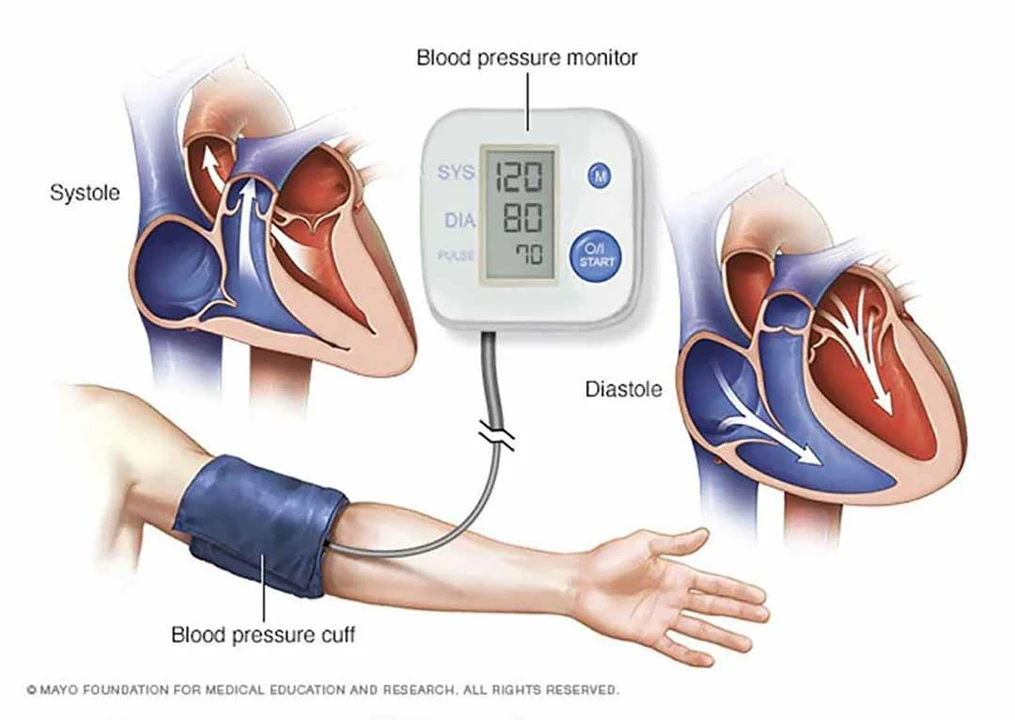
A hypertensive crisis happens when blood pressure shoots dangerously high — usually systolic over 180 mmHg or diastolic over 120 mmHg. That number alone is a red flag, but what matters more is whether organs are being damaged. This can go from 'I feel awful' to life-threatening in hours, so quick action matters.
How to recognize it fast
There are two types: hypertensive emergency and hypertensive urgency. With an emergency, organ damage is happening now. Look for severe headache, chest pain, shortness of breath, confusion, sudden weakness or numbness, vision changes, or vomiting. If you or someone has any of these with very high BP, call emergency services immediately.
Hypertensive urgency means the pressure is very high but there’s no clear organ damage yet. You might feel really anxious, have a pounding headache, or notice nosebleeds. It still needs prompt medical attention, but it’s handled differently than an emergency.
What to do right away
If you suspect a hypertensive crisis, don’t wait. Call 911 or go to the nearest emergency room. While waiting, have the person sit down and stay calm—stress and activity can make blood pressure climb higher. If they take prescribed BP meds, encourage them to take them exactly as directed, but don’t double doses. If they’re confused or vomiting, don’t force pills by mouth.
Avoid painkillers, herbal remedies, or stimulants like caffeine or nicotine. If someone is losing consciousness or having a seizure, follow basic first aid and tell the EMTs about all meds, recent changes, and any drug use. That info helps doctors choose safe treatments.
In the ER, expect monitoring and tests: repeated BP readings, blood tests, ECG, chest X-ray, and possibly CT scans if stroke or aortic dissection is suspected. For hypertensive emergency, doctors usually give IV antihypertensive drugs (examples commonly used include labetalol, nicardipine, or nitroprusside) to lower pressure slowly and safely. Dropping pressure too fast can hurt the brain and other organs, so controlled reduction is the goal.
Common causes include stopping BP meds suddenly, bad interactions with other drugs, severe pain, illicit stimulants, pregnancy-related conditions like preeclampsia/eclampsia, and certain endocrine issues. Long-standing uncontrolled hypertension raises the risk too.
After the crisis is managed, you’ll get a clear plan: which meds to take, follow-up with a primary care doctor or cardiologist, and lifestyle steps to prevent recurrence—salt control, regular meds, weight target, and avoiding risky substances. If you've had a hypertensive crisis before, keep a current list of medications and emergency contacts on you.
Quick tip: if you have a home BP monitor, bring recent readings to the ER. That snapshot helps doctors see trends and make better decisions fast.