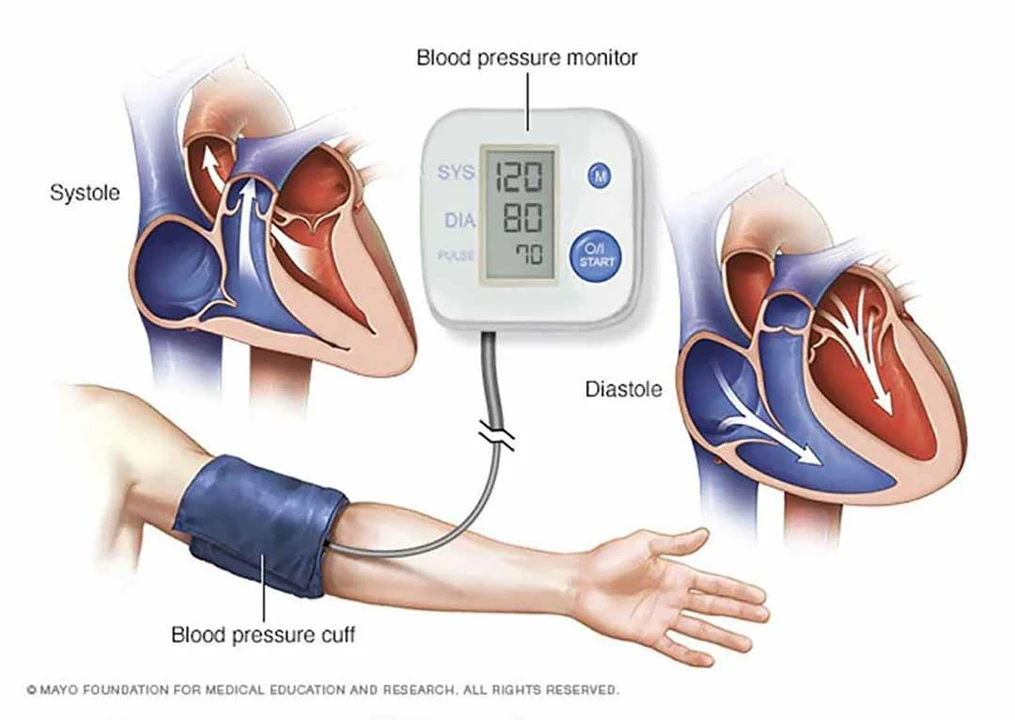
Blood pressure: what the numbers really mean and what to do
High blood pressure often feels normal until it isn't. Many people have elevated numbers for years with no symptoms, then face a stroke, heart attack, or kidney trouble. Knowing your numbers and acting on them is the fastest way to cut risk.
How to measure blood pressure at home
Use an automatic upper-arm monitor that has been validated. Sit quietly for 5 minutes, feet flat, back supported, arm at heart level. Take two readings 1 minute apart and record both; repeat morning and evening for a week to get a reliable baseline. Make sure the cuff fits—too small or too large gives wrong results.
Understand the categories: normal is under 120/80 mmHg. Elevated is 120–129/<80. Stage 1 hypertension is 130–139/80–89. Stage 2 is 140/90 or higher. If readings spike above 180/120, get medical help right away.
Simple changes that lower your numbers
Small, consistent habits move the needle. Aim for these practical steps you can start this week:
- Cut added salt: shoot for under 2,300 mg daily; 1,500 mg helps more if you have high BP. Cook with herbs and lemon instead of salt.
- Move more: 30 minutes of brisk walking most days (about 150 minutes per week) lowers pressure and improves weight.
- Lose 5–10% of body weight if overweight—each kilo lost often drops BP a little.
- Eat more potassium-rich foods: bananas, beans, spinach, potatoes. Potassium helps balance sodium.
- Limit alcohol: keep it to one drink a day for women, two for men, and avoid binge drinking.
- Sleep and stress: aim for regular sleep and try simple stress tools—breathing, short walks, or 10 minutes of guided relaxation.
These changes can cut systolic pressure by 4–11 mmHg on average, enough to matter for many people.
Medications are common and safe when used properly. Common drug classes include ACE inhibitors, ARBs, thiazide diuretics, calcium channel blockers and beta-blockers. Your doctor picks one based on your age, other conditions, and side effects. Never stop a prescribed drug suddenly—talk with your clinician to adjust doses or switch medicines.
Keep a log of home readings and take it to appointments. Home values often differ from office checks; doctors use both to decide treatment. If your readings stay high despite lifestyle changes and pills, your clinician may check for secondary causes like sleep apnea, thyroid issues, or certain medications that raise pressure.
Want a quick plan? Get a validated home monitor, track twice daily for a week, cut salt and alcohol, walk 30 minutes five times this week, and book a check-up with your doctor with your log. Small steps add up fast—start with one and build from there.